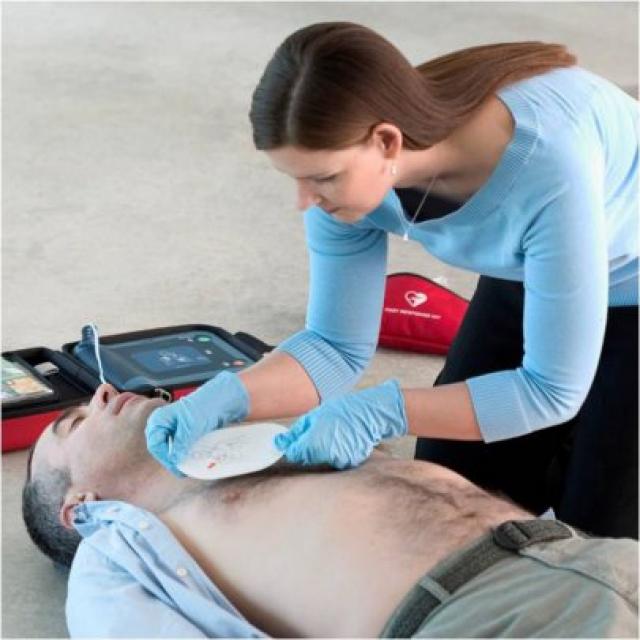
AED stands for Automated External Defibrillator.
How does an AED work?
The heart has its own natural pacemaker: the SA node, which is located in the right upper chamber (atrium) of the heart. It fires an electric burst in a rhythmic pattern to stimulate your heart to beat.
Cardiac arrest occurs when this electrical system fails—and the steady rhythm of your heartbeat stops. When that occurs, an AED delivers an electrical charge that can restart the heart’s electrical system.
An AED is a lightweight, portable device with a built-in computer and adhesive electrodes that can be attached to a victim’s chest. The rescuer attaches the electrodes, and through these the AED analyzes the victim’s heart rhythm to determine whether an electric shock is needed.
If it is, the rescuer presses the button to deliver the shock to the victim’s heart—stimulating it to assume its normal rhythm.
AEDs are medically sophisticated equipment, but they’re designed to be used by anyone, whether or not you have any medical training. It provides clear, easily understood directions that can be followed by non-medical professionals.
While many CPR training programs include training in the use of an AED—ours does—you don’t need to have training in order to use one. They’re that easy to use.
What do AEDs detect?
AEDs are designed to recognize two types of abnormal heart rhythms: ventricular fibrillation and ventricular tachycardia. Both are caused by a misfiring in the electrical signal that keeps the heart pumping normally.
Ventricular tachycardia occurs when the heart beats faster than normal. Ventricular fibrillation occurs at the extreme end of that—where the heartbeat becomes so rapid and chaotic that the heart walls quiver uselessly, losing their ability to pump blood.
Both types of heart arrhythmia reduce the heart’s ability to pump blood. This cuts the amount of oxygen the heart gets, and impairs its ability to pump blood even further. It’s a vicious cycle. Both types of arrhythmia can result in cardiac arrest and death.
The AED recognizes both types of arrhythmia and will deliver a shock to stop the heart—halting the irregular electrical signal. This gives the heart a chance to reset itself and, hopefully, start up a normal, rhythmic heartbeat again.
The AED can be crucial to saving lives—because the more time lapses without oxygenated blood circulating in the body, the more the heart, brain, and other organs are damaged.
For every minute an arrhythmic heart does not get defibrillated, the chances of the patient’s survival go down by 10%. If the patient gets defibrillated early enough, their chances of survival go up to 50% or higher.
What to expect when using an AED
When using an AED, some precautions should be taken. While you can safely deliver a shock in rain, snow, or on a damp surface, it’s best not to try it while the victim is lying in standing water—like a kiddie pool or bathtub—or on a metal surface.
Most AEDs are designed to be used on full-sized adults, or children aged 8 or older who weigh more than 55 pounds.
Not every AED is the same. There are a number of different manufacturers, so there are variations between different models. However, the concept is the same, and they’re all designed to be very intuitive and easy to use in an emergency.
Steps to using an AED
The AED will deliver step-by-step instructions through voice prompts, text messages, and lights. Here are the steps for using an AED:
- Turn on the machine, either by opening the lid or pressing the “On” button.
- Take the patient’s shirt off. Make sure their skin is dry. Thick chest hair may need to be shaved.
- Place an electrical pad on the upper right side of the chest, above the nipple.
- Place an electrical pad on the lower left, on the ribs under the armpit.
- Press both pads down so they’re firmly attached.
- Follow the prompts from the AED. This is the point where the machine will analyze the victim’s heart rhythm to decide if a shock is needed.
- If a shock is needed, the AED will say “Shock advised, charging.” Shout “Clear” and be sure no one is touching the victim.
- The AED will tell you when to press the button and deliver a charge. Follow the instructions.
- Deliver CPR after the shock. If the AED doesn’t advise you to shock the victim, deliver CPR as long as the victim is not moving or breathing.
- Keep the pads on the patient’s body. Every two minutes, the machine will reassess the victim’s heartbeat. It may tell you to shock the victim again.
Statistics and facts about AEDs
- Approximately half a million people are struck down by sudden cardiac arrest every year.
- Of those, approximately 395,000 suffer sudden cardiac arrest per year outside of a hospital setting.
- Sudden cardiac arrest can strike anyone of any age. You do not need to have any prior history of heart troubles to be a victim of cardiac arrest.
- Only about 6% of people stricken with cardiac arrest outside of a hospital survive.
- However, of those who receive defibrillation from an AED within the first minute, the survival rate is 90%.
- The survival rate of sudden cardiac arrest is 30-50% for those who receive defibrillation within the first five minutes.
- For every minute that a cardiac arrest victim does not receive defibrillation, the chances of survival decrease by 7-10%.
- Half of all workers do not know where the AED is at their workplace. In the hospitality industry, that number is 66%.
Because cardiac arrest occurs so frequently outside of hospitals, it’s crucial for AEDs to be accessible in public places—and for bystanders to be willing to use them. AEDs are easy for anyone to use, even those with no medical training—but getting trained in AED use can give you the confidence to use one if needed. That’s why we recommend it.
Sign up for a class at CPR Tally, Tallahassee’s leading premier training site for the American Heart Association. Our website is www.cprtally.com with upcoming classes every week or give us a call at (850) 559-1678.
